Guest article by
Mich Powers, DVM, CCRT
Diplomate of the American College of Veterinary Surgeons -SA
Diplomate of the American College of Sports Medicine & Rehabilitation (canine)
See Part I – The Benefits of PennHIP and the physical exam
Start with Patient History
It is important to obtain a thorough history of the patient. Note if this is a chronic lameness, acute on chronic, or a new finding. Confirm which leg or is it a switching leg lameness. Watch for non-specific signs such as exercise intolerance, difficulty rising or lying down, avoidance or difficulty of stairs, or jumping into the car or onto furniture. This is especially important to localize the current issue and not just attribute a hind end lameness in a dog that has a history of hip dysplasia. Clinical signs of hip dysplasia in older patients are most often gradual and progressive; therefore an adult patient presenting for acute onset of hind limb lameness attributed to hip dysplasia should be carefully screened for other conditions.
Check Signalment
Age
CHD is a juvenile-onset condition, but we see two recognizable clinical groups of dogs:
1. Acute (severe) phase seen in young dogs 4-12 months of age. Signs tend to be by acute onset and are typically more severe with pain of hips being quite common. The pain is thought to be caused by stretching and tearing of joint capsule and other supporting structures, along with acetabular microfracture. (Piermattei DL, 2006) Clinical signs observed: Lameness, low exercise tolerance, reluctance to climb stairs or jump into cars, difficulty lying down or rising, an audible “click” when walking, or narrow base stance. Potentially positive Ortolani test.
2. Chronic (mild) phase seen in older dogs over 15 months of age. The reasons we may not see these groups of dogs at a younger age could be due to: unnoticed signs by the owner, undiagnosed by the veterinarian, and/or some dogs may not exhibit clinical signs until later in the disease process, often correlated with progression of osteoarthritis. This patient population can exhibit clinical signs like younger patients but clinical signs in older patients are often more due to osteoarthritic changes that have occurred, rather than signs associated with laxity and subluxation.
An affected dog of either group may have one or any combination of the following clinical signs:
Clinical signs of Hip Dysplasia
| General Signs | Hind Limb Clinical Findings | Gait Analysis |
|---|---|---|
| Exercise intolerance | Pain on palpation of hips | Hind end sways when walking |
| Reluctance to navigate stairs | Hind limb muscle atrophy | Ataxic-appearing gait, with normal neurologic examination |
| Difficulty lying down or rising | Limited range of motion | Walking with an arched back |
| Audible click or clunk when walking | Positive OrtolaniVideo: Ortolani exam to test for hip laxity sign | Base-narrow stance of the hind limbs |
| Lameness uni- or bilateral | Clicking or clunking sound | Bunny hopping |
| Crepitus on hip palpation | Bilateral or unilateral hind limb lameness |
Breed Risk
Any size or breed of dog can be affected with hip dysplasia, but it is most diagnosed in large and giant breed dogs. Breeds with the most evaluations by the Orthopedic Foundation for Animals (OFA) for hip dysplasia over the last 45 years include Labrador Retrievers, Golden Retrievers, and German Shepherds. The range of percentage of excellent hip evaluation and percentage of dysplastic reported over the last 15 years in the 3 most reported breeds to the OFA:
3 Most Reported Breeds for Hip Dysplasia
| Breed | % with Excellent Hip Evaluations | % of Dysplastic Evaluations |
|---|---|---|
| Labrador Retrievers | 24.9 – 31.8 | 8.9 -13.3 |
| Golden Retrievers | 8.6 -11.5 | 15.4 – 26.8 |
| German Shepherds | 7.1 -7-4 | 18.6 -31.4 |
Breeds with particularly high reported prevalence of dysplasia to OFA include the Pug, Bulldog and St. Bernard.
| Breed | % with Excellent Hip Evaluations | % of Dysplastic Evaluations |
|---|---|---|
| Pug | 0 -1.6 | 80.4 -103.2 |
| Bulldog | 0 -0.7 | 60.3 – 88.7 |
| St. Bernard | 3.6 – 6.6 | 41.9 - 90 |
These numbers though do not indicate a true prevalence of dogs in the OFA database because films are not required to be submitted, it is up to the owner of the patient to decide. In a study evaluating submission bias, it was found that 92% of dogs with dysplastic hips were not submitted to the OFA for evaluation; however, 50% of normal dogs were also not submitted, suggesting that this bias occurs in both directions. (Paster ER, 2005)
Although certain dog breeds are predisposed, mixed-breed dogs can also develop hip dysplasia.
Sex
There have been multiple large prevalence studies that show no sex predilection associated with hip dysplasia. (Runge JJ, 2010) However, a study by Witsberger et al. (Witsberger TH, 2008) showed that males are more at risk for CHD. Some studies suggest that male neutered dogs may be at increased risk for the development of hip dysplasia, especially when neutered early. (Witsberger TH, 2008)
Physical Exam
Your physical exam should include:
- Lameness Evaluation
- Gait abnormalities (noted in the first table in this article) can be seen on examination. Hip dysplasia/OA is typically a bilateral condition, but you can see clinical signs are more severe on one side and even a unilateral lameness may be appreciated.
- Orthopedic Examination
- A complete general physical examination should be performed both to rule out other disease processes and the overall health of the patient. A systematic orthopedic examination should localize discomfort to the hips. Common clinical signs seen are listed in Table 1.
For dysplastic patients, hip manipulation is typically painful, particularly hip extension. Pain on hip extension must be differentiated from other conditions. Common differential diagnoses for pain localized to the hip region are iliopsoas strain, slipped capital femoral physis, Legg-Calvé-Perthes disease, osteochondrosis, lumbosacral disease, and neoplasia. In addition to hip pain, patients with advanced osteoarthritis may also exhibit crepitus on palpation of the hip, as well as decreased coxofemoral range of motion and muscle atrophy of the affected limb.
Other observations and findings include:
- While standing, is the dog shifting body weight to the left, to the right, or rostrally to the forelimbs?
- When positioning to lie down, does the dog tuck his legs under and to one side, using their forelimbs to guide themselves into a down?
- When going to get up from a lying-down position, do they throw weight forward and pull up with their forelimbs?
- Muscling of the hind limbs should be evaluated. Is the hind end muscling equal and symmetrical and does it seem appropriate for the size of the dog? Do they have a “skinny” back end and more front end loaded?
- Does the dog sit square?
Complete orthopedic evaluation is critical because comorbidities may be present that complicate treatment recommendations. For example, an adult dog presenting with acute-onset hind limb lameness may indeed have hip dysplasia with severe OA, but the lameness may be attributable to another common cause of lameness of the hind a cranial cruciate ligament rupture (CCLR).
Interpreting your radiographic results
There have been multiple studies showing there is no relationship between limb function and the severity of radiographic signs. (Gordon WJ, 2003) The osteoarthritic joint does not correlate to the amount of clinical discomfort a dog has.
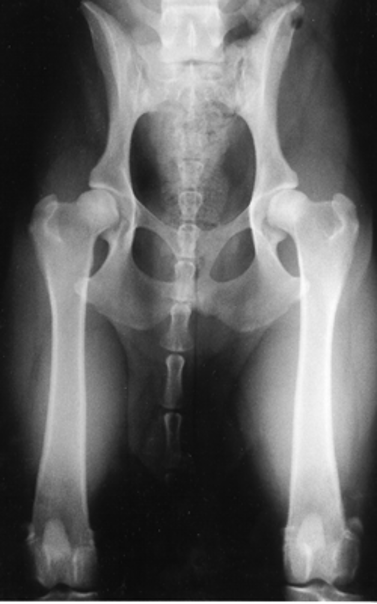
The hip extended ventrodorsal pelvic radiograph’s main advantage is that it gives one the ability to evaluate the joint for signs of osteoarthritis. Radiographic evidence of osteoarthritis of the coxofemoral joint includes femoral periarticular osteophyte formation, subchondral sclerosis of the craniodorsal acetabulum, osteophytes along the acetabular margin, and joint remodeling.
PennHIP distraction index is the most reliable indicator of future hip osteoarthritis, can be done as early as 16 weeks of age. 80% of dogs evaluated as “normal” by the OFA (hip -extended view) were found to have hip laxity by PennHIP testing that predisposed them to developing hip osteoarthritis in the future. (Powers MY K. G., 2010) PennHIP will enable you to guide owners on what types of activities are more suited. Will he be able to be a working or agility dog? How does the dog compare to its breed and should the dog be used for breeding? These are questions that a PennHIP evaluation can give you to help you to educate your owners on the risk of getting hip OA, managing CHD, and types of activities the dog can do.
CHD vs. other orthopedic and neurologic disorders
Canine hip dysplasia is considered the most common orthopedic condition diagnosed in the dog, but most patients have only mild clinical signs associated with CHD. Other neurologic and orthopedic diseases, especially cranial cruciate ligament ruptures (CCLR) are likely the most common hind end lameness we are now seeing. (Powers MY M. S., 2005)
Dogs with stifle, hip, or lower back pain will present with remarkably similar signs such as difficulty rising, tucking the hind end when sitting, and usually placing their limbs to one side instead of sitting square, avoidance or difficulty in getting into an automobile, getting on furniture or doing stairs. In addition, musculoskeletal injuries especially to the iliopsoas muscle (which generally is a compensatory injury) can cause a change in lameness in a dog with CHD.
Dogs with CHD and OA, as they get older, their clinical signs are generally static over the years. A “weekend warrior syndrome” may cause a flare-up but generally, it’s an overall hind end soreness with potential one side being worse than the other, but generally resolves back to their “normal” within a few days.
When a dog is presenting for an acute hind limb lameness or lameness that is now progressing, exclusion of other orthopedic and neurologic diseases is paramount. Many times, veterinarians will assume the lameness is due to the hip OA, especially seeing the radiographic changes in the hip. It is important to remember that radiographic changes do not correlate to clinical signs.
A previous study (Powers MY M. S., 2005) showed that in dogs referred to a veterinary teaching hospital for hip discomfort, 32% of the hind end lameness was due to CCLR. Of the dogs diagnosed with CCLR, 94% had radiographic signs of CHD, but 92% had stifle joint effusion, and 81% had a cranial drawer sign. The average age of dogs having CCLR use to be 7-8yr of age, we now are seeing dogs much younger in age. The mean age in the study was 3.8 yrs of age. Due to the high prevalence of CCLR in dogs referred for lameness because of CHD, it is important to exclude other sources of stifle joint disease before making recommendations for treatment of CHD.
Comorbidities are common, especially as the patient ages. Disorders of the hip, stifle and neurologic disease can mimic the clinical signs of CHD. For example, a dog with lumbosacral (LS) disease will have an ataxic gait, resist jumping up on furniture, and pain on hip extension because there is hyperextension of the lumbosacral region when extending out the hips. Therefore, it is imperative to rule out other causes of hind end lameness or note that the dog may have multiple co-morbidities.
| Stifle | Hips | LS Disease | |
|---|---|---|---|
| Difficulty rising | Y | Y | Y |
| Avoidance jumping up | Y | Y | Y |
| Difficulty lying down or sitting | Y | Y | Y |
| Stiff short strided gait | Y | Y | Y |
It is not uncommon for an older hip dysplastic dog to have LS disease and cranial cruciate ligament rupture (CCLR). Hence, it is important to discuss with owners that yes, your dog has hip OA but is now lame due to CCLR, and stabilizing the CCLR is recommended. It’s important that they understand that there still could be lameness or flare-ups after cruciate surgery due to the other co-morbidities.